This guide shares 10 essential thalassemia management tips, including diet, treatment adherence, lifestyle habits, regular monitoring, and emotional support. It helps improve daily health, prevent complications, and enhance quality of life for patients living with thalassemia.
Understanding Your Thalassemia Diagnosis and Care Plan
When it comes to thalassemia management, the foundation is a clear understanding of your specific subtype and personalized treatment regimen. Thalassemia ranges from trait forms—often referred to as minor—to more severe intermedia and major variants. Accurate diagnosis typically involves genetic testing and a detailed review of hemoglobin levels. Engaging with a hematologist who specializes in hemoglobinopathies ensures that your blood counts, iron indices, and organ function are monitored closely.
Collaborative Care with Hematology Specialists
Developing a solid partnership with your healthcare team empowers you to make informed decisions. Keep a centralized record of lab results, transfusion dates, chelation schedules, and any side effects. Digital tools or mobile apps can streamline data logging, enabling trend analysis and timely adjustments. During consultations, ask pointed questions about target hemoglobin thresholds and optimal chelation dosing. For reputable guidelines on transfusion targets, refer to resources like the National Heart, Lung, and Blood Institute (NHLBI).
Interpreting Diagnostic Tests and Genetic Counseling
Periodic assessments of serum ferritin and liver iron concentration guide chelation therapy adjustments. Understanding how to interpret these values allows you to recognize warning signs of iron overload early. Moreover, genetic counseling offers valuable insights into inheritance patterns, family planning, and prenatal testing options. Consulting a board-certified genetic counselor can clarify what the results mean for you and your relatives.
Building Your Thalassemia Action Plan
Create a personalized action plan that outlines transfusion frequency, chelation administration, dietary goals, and emergency contacts. Share this document with family members, caregivers, and local healthcare providers to ensure seamless care continuity, especially when traveling or during natural disasters. In today’s landscape, storing a digital copy on secure cloud platforms enhances accessibility in urgent situations.
Optimizing Nutrition to Support Red Blood Cell Production

Nutrition and Dietary Strategies in Thalassemia Management
A well-planned, nutrient-rich diet is a key component of effective thalassemia management. While food alone cannot replace medical treatment, it plays an important supportive role in improving energy levels, enhancing red blood cell production, and reducing oxidative stress. Working closely with a registered dietitian ensures that dietary choices are aligned with iron levels, treatment plans, and individual health needs.
Balancing Iron Intake and Chelation Therapy
In thalassemia management, controlling iron levels is essential, especially for patients undergoing regular transfusions.
Key Dietary Considerations:
- Include moderate amounts of iron-rich foods when recommended
- Monitor intake of red meat, legumes, spinach, and fortified cereals
- Coordinate diet with iron chelation therapy (e.g., deferasirox, deferiprone)
- Avoid excess iron accumulation through regular medical supervision
Monitoring:
- Serum ferritin tests every 3–4 months
- Adjust diet based on iron overload status
- Continuous coordination with healthcare providers
Enhancing Iron Absorption Safely
Improving nutrient absorption is important, especially from plant-based sources.
Best Practices:
- Combine plant iron sources with vitamin C-rich foods
- Add citrus fruits, strawberries, or bell peppers to meals
- Use lemon juice with leafy greens or lentil-based dishes
- Maintain a colorful and diverse diet for better nutrient intake
Supporting Red Blood Cell Formation
Proper nutrition supports hematopoiesis and overall blood health in thalassemia management.
Essential Nutrients:
- Vitamin B12: eggs, dairy, poultry
- Folate: leafy greens, asparagus, whole grains
- Balanced protein intake for tissue repair and energy
Medical Guidance:
- Supplements only under physician supervision
- Regular monitoring for deficiencies or absorption issues
Hydration and Electrolyte Balance
Adequate hydration is crucial for circulation and overall well-being in thalassemia management.
Recommendations:
- Drink 8–10 glasses of water daily
- Increase fluid intake during heat or physical activity
- Use electrolyte-rich foods like bananas, yogurt, and sweet potatoes
- Maintain balance to prevent fatigue and cramps
Managing Iron Overload and Transfusion Protocols in Thalassemia Management
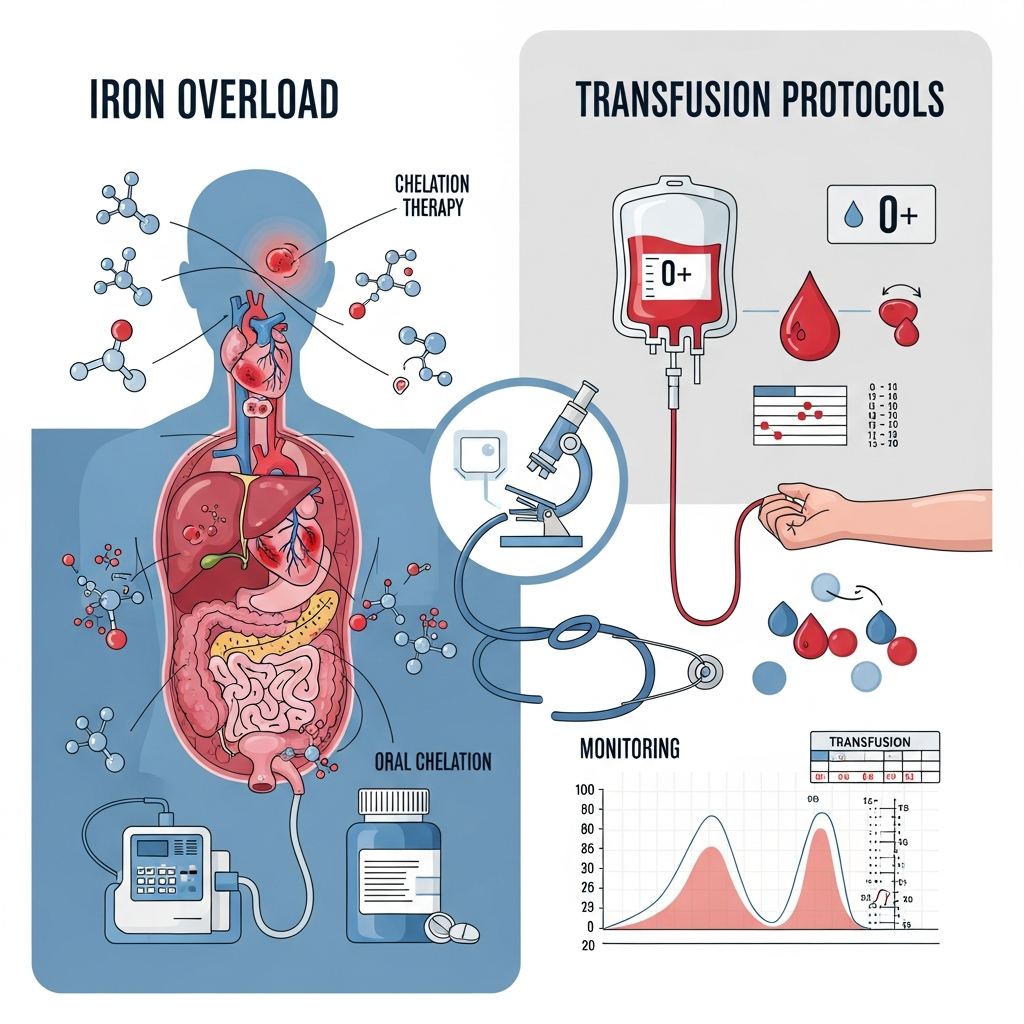 A key challenge in long-term thalassemia management is controlling iron overload caused by repeated blood transfusions. While transfusions are essential for maintaining healthy hemoglobin levels, excess iron can gradually accumulate in vital organs such as the heart, liver, pancreas, and endocrine glands, leading to serious complications if not properly managed.
A key challenge in long-term thalassemia management is controlling iron overload caused by repeated blood transfusions. While transfusions are essential for maintaining healthy hemoglobin levels, excess iron can gradually accumulate in vital organs such as the heart, liver, pancreas, and endocrine glands, leading to serious complications if not properly managed.
Understanding Iron Overload in Thalassemia Management
Regular transfusions introduce more iron than the body can naturally eliminate. Without proper control, this excess iron becomes toxic over time.
Major Risks:
- Heart damage (cardiomyopathy)
- Liver fibrosis and cirrhosis
- Endocrine disorders (diabetes, hormone imbalance)
- Pancreatic dysfunction
Effective thalassemia management requires early detection and continuous monitoring of iron levels.
Chelation Therapy and Medication Adherence
Chelation therapy is the cornerstone of iron control in thalassemia management.
Common Chelators:
- Deferoxamine – subcutaneous infusion
- Deferasirox – once-daily oral tablet
- Deferiprone – multiple daily oral doses
Best Practices:
- Take medications exactly as prescribed
- Use reminders or mobile apps for adherence
- Never skip doses without medical advice
- Report side effects promptly to healthcare providers
Consistent use is essential to prevent long-term organ damage.
Monitoring Iron Levels and Organ Function
Regular testing helps ensure safe and effective thalassemia management.
Key Monitoring Tools:
- Serum ferritin every 3 months
- Liver iron concentration via MRI
- Cardiac T2* MRI for heart iron load
- Echocardiograms for heart function
Clinical Importance:
- Early detection of iron overload
- Timely adjustment of chelation dosage
- Prevention of irreversible organ damage
For safety guidelines, consult trusted health authorities such as the CDC.
Post-Transfusion Care and Recovery
Proper care after transfusion is an important part of thalassemia management.
Post-Transfusion Guidelines:
- Rest for 24–48 hours after transfusion
- Monitor for fever, chills, or allergic reactions
- Stay hydrated to support circulation
- Keep a symptom diary for follow-up visits
When to Seek Help:
- Sudden chest pain or breathing difficulty
- High fever or severe fatigue
- Unusual swelling or pain
Implementing Safe Exercise and Hydration Strategies
 Regular physical activity is an important part of thalassemia management, supporting heart health, bone strength, circulation, and mental well-being. However, since individuals with thalassemia often experience anemia-related fatigue, exercise must be carefully planned to avoid overexertion and maintain safe energy levels.
Regular physical activity is an important part of thalassemia management, supporting heart health, bone strength, circulation, and mental well-being. However, since individuals with thalassemia often experience anemia-related fatigue, exercise must be carefully planned to avoid overexertion and maintain safe energy levels.
Choosing Safe Low-Impact Exercises in Thalassemia Management
Low-impact workouts are ideal for maintaining fitness without placing excessive stress on the body.
Recommended Activities:
- Walking at a steady, comfortable pace
- Swimming for full-body, low-stress movement
- Yoga for flexibility and stress relief
- Stationary cycling for cardiovascular health
Exercise Guidelines:
- 20–30 minutes per session
- 3–5 times per week
- Moderate intensity (50–70% heart rate)
- Adjust based on fatigue levels
Key Principle:
In thalassemia management, consistency is more important than intensity.
Timing Exercise with Transfusion Cycles
Energy levels fluctuate depending on transfusion schedules, making timing an important part of thalassemia management.
Best Practice:
- Schedule more intense workouts 5–7 days after transfusion
- Perform light stretching or yoga before the next transfusion cycle
- Avoid strenuous exercise during low hemoglobin periods
Benefits:
- Maximizes energy efficiency
- Reduces fatigue risk
- Improves exercise tolerance safely
Hydration and Electrolyte Balance in Thalassemia Management
Proper hydration is essential during physical activity to prevent complications.
Hydration Tips:
- Drink water before, during, and after exercise
- Increase intake in hot or humid weather
- Use electrolyte drinks for longer sessions
- Include potassium- and magnesium-rich foods
Important Notes:
- Dehydration can worsen fatigue and dizziness
- Fluid needs should be personalized with medical guidance
Supporting Emotional Well-Being and Emergency Preparedness in Thalassemia Management
A complete thalassemia management tips plan goes beyond medical treatment and includes emotional health, crisis planning, and long-term life preparedness. Living with a chronic condition can be challenging, and emotional resilience plays a key role in maintaining treatment adherence and overall quality of life.
Mental Health and Emotional Support in Thalassemia Management
Emotional well-being is a vital part of effective thalassemia management, helping patients cope with stress, fatigue, and long-term treatment routines.
Key Strategies:
- Daily mindfulness and deep breathing exercises
- Meditation or relaxation techniques for stress reduction
- Cognitive Behavioral Therapy (CBT) for emotional support
- Participation in peer support groups and online communities
Community Support:
Organizations like patient associations and global thalassemia networks help patients stay informed, connected, and empowered.
Emergency Preparedness in Thalassemia Management
Unexpected situations can interrupt treatment, making preparedness essential in thalassemia management.
Emergency Kit Should Include:
- Recent blood transfusion records
- Lab reports and ferritin levels
- Medication and chelation schedule
- Allergy and medical alerts
- Emergency contact list
Additional Tips:
- Keep both printed and digital copies of medical records
- Store files securely in cloud storage
- Update information regularly
Travel Safety and Planning in Thalassemia Management
Careful planning ensures safe travel without disrupting treatment.
Travel Checklist:
- Locate nearby transfusion centers before travel
- Carry physician’s medical summary letter
- Confirm insurance coverage for medical care
- Pack enough chelation medication for the trip duration
- Check pharmacy availability at destination
Family Planning and Genetic Counseling
Genetic counseling is an important preventive aspect of thalassemia management, especially for individuals planning a family.
Key Considerations:
- Understand inheritance patterns (autosomal recessive)
- Access prenatal tests like CVS or amniocentesis
- Evaluate partner carrier status
- Plan pregnancies under specialist supervision
Emergency Preparedness Overview Table
| Area | Preparation Strategy | Purpose |
|---|---|---|
| Mental Health | Therapy, mindfulness, support groups | Reduce stress and improve coping |
| Medical Records | Digital + physical copies | Ensure continuity of care |
| Travel Planning | Identify hospitals & carry prescriptions | Prevent treatment disruption |
| Insurance | Verify coverage before travel | Avoid financial barriers |
| Genetic Counseling | Carrier screening & prenatal testing | Informed family planning |
Frequently Asked Questions
1. What is thalassemia management?
Thalassemia management refers to the comprehensive care approach that includes transfusions, iron chelation, diet, lifestyle support, and regular monitoring to control symptoms and prevent complications.
2. Why is emotional support important in thalassemia management?
Emotional support helps reduce stress, anxiety, and depression, improving treatment adherence and overall quality of life for patients.
3. What are the best exercises for thalassemia patients?
Low-impact activities like walking, swimming, yoga, and cycling are recommended to improve fitness without causing excessive fatigue.
4. How often should thalassemia patients get blood transfusions?
Severe cases typically require transfusions every 2–4 weeks, depending on hemoglobin levels and medical guidance.
5. What is iron overload in thalassemia?
Iron overload occurs due to repeated transfusions, leading to excess iron buildup in organs like the heart and liver if not managed with chelation therapy.
6. What foods should be included in a thalassemia diet?
A balanced diet rich in folate, vitamin B12, vitamin C, calcium, and protein is recommended to support overall health.
7. Why is chelation therapy necessary?
Chelation therapy removes excess iron from the body and prevents long-term organ damage caused by transfusions.
8. Can people with thalassemia travel safely?
Yes, with proper planning, medication, medical records, and access to transfusion centers, travel is safe for most patients.
9. Is thalassemia curable?
Currently, stem cell transplantation is the only established cure, while gene therapy is an emerging treatment option.
10. Why is genetic counseling important in thalassemia?
Genetic counseling helps families understand inheritance risks and make informed decisions about pregnancy and prenatal testing.
Conclusion
Optimal thalassemia management demands a proactive, multifaceted approach. By gaining in-depth insight into your diagnosis, collaborating closely with hematology experts, and meticulously logging lab results, you establish a strong medical foundation. Nutrient-rich meals, strategic hydration, and safe exercise routines boost resilience, while vigilant iron overload monitoring and chelation adherence protect critical organs. Equally important is nurturing mental health through community connections, mindfulness, and emergency preparedness. As you implement these five core pillars, remember that incremental daily choices accumulate into substantial long-term benefits. Lean on authoritative resources such as the CDC and NHLBI, maintain open communication with your healthcare team, and adapt strategies to fit your evolving needs. With knowledge, preparation, and support, you can thrive with thalassemia and enjoy a vibrant, fulfilling life.


